Our Blog
When Chronic Pain Becomes Too Much: Understanding the Link Between Physical and Mental Health
January 31, 2024
It’s something we’ve all experienced before: that sluggish, exhausted, “don’t want to get out of bed this morning” feeling. Maybe you had a late night or are fighting off a cold. Maybe it’s just the dreary weather. You have things to do, though, so you drag yourself up and start your day.
For many people, this kind of morning is the best they will ever feel … the most they could hope for from their day. This is what it’s like living with physical illness and chronic pain, and they can have a significantly negative effect on a person’s mental health.
The connection between physical and mental health is well-established. According to the American Psychiatric Association, people living with chronic pain are at increased risk for mental illness, especially depression, anxiety, and substance use disorders. And since chronic pain is often invisible to the naked eye, sufferers find themselves feeling misunderstood — or worse, not believed — by the people they care about, leading to isolation and further perpetuating a cycle of mental instability.
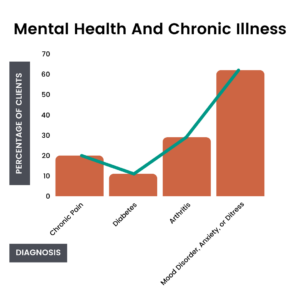 This link between chronic pain and mental illness is something we see daily at Guild. Last year, 20 percent of our clients told us they dealt with chronic pain, 11 percent were diagnosed with diabetes, 29 percent had been diagnosed with arthritis, and 62 percent had a diagnosed mood disorder or suffered from generalized anxiety or distress.
This link between chronic pain and mental illness is something we see daily at Guild. Last year, 20 percent of our clients told us they dealt with chronic pain, 11 percent were diagnosed with diabetes, 29 percent had been diagnosed with arthritis, and 62 percent had a diagnosed mood disorder or suffered from generalized anxiety or distress.
It’s a “chicken or the egg” scenario, in which it’s nearly impossible to know what causes what. Did the mental illness come first, or the physical pain? Research in this area has been largely unclear so far, with studies suggesting both could be true. According to the Centers for Disease Control and Prevention, depression can increase the risk for physical health problems like diabetes, heart disease, and stroke, while chronic illness can increase the risk for mental health problems.
At Guild, we know it’s crucial to take into account both a person’s mental and physical health when putting together a treatment plan, especially during or shortly after a mental health crisis.
“We do everything we can to help our clients build an infrastructure of physical health around them,” says Doreen Rusk, program manager for our Scott County Residential Center. “Our staff frequently use walks with our clients as a part of their support and care, and making doctors appointments and providing culinary and nutrition classes are additional ways we look to help their physical and mental recovery.”
The link between physical activity and improved mental health is something our staff understand well and utilize when working with clients.
“It’s a bidirectional influence on each other that we have to address,” Rusk says. “When we improve our physical health, it impacts our mental wellness, and when we work on our mental health, it makes it easier to get up and move our bodies. Our residential center has a courtyard where our clients can go out to get fresh air, and we have a workout room with stationary bikes, weights, and yoga mats to use.”
Combining Guild’s person-centered care approach with all that we know about chronic illness enables holistic treatment for our clients living with mental illness. This intersectional approach helps us create the tools, spaces and supports that counter the isolated and painful experiences that living with physical illness, chronic pain and mental illness can bring. The approach is ultimately how we help our clients thrive.
“There is immense impact on our physical health when we begin looking forward to things again,” Rusk says.
